Antibiotic Resistant Sexually Transmitted Infections (STIs)
Sexually transmitted infections (STIs) are infections that usually occur through sexual contact. The organisms (bacteria, viruses or parasites) that cause STIs may pass from one person to another in the blood, semen or vagina and other body fluids. Sometimes these infections can occur non-sexually, for example, during pregnancy and childbirth or through sharing needles.
Some of these STIs caused by bacteria have proved resistant to many of the commonly used antibiotics. These would be known as drug resistant STIs. Symptoms may not always be present with STIs, therefore it is possible that STIs, including resistant STIs, can be transmitted from people who appear healthy and show no signs of infection.
Who is at risk from antibiotic-resistant sexually transmitted infections?
People at the greatest risk of antibiotic resistant infections are often living with underlying medical conditions. They may also have weakened immune systems due to illness or as a side effect of treatment for their condition.
People can also be affected by antibiotic-resistant sexually transmitted infections (STIs) if they practise unprotected sex or have sex with multiple partners. Unprotected sex means that they do not use a condom. People who inject drugs or those that have a history of STIs may develop on-going or repeated antibiotic resistant STIs.
The biggest risks with untreated or on-going antibiotic resistant STIs include infertility, pelvic pain, and pregnancy complications.
What type of bacteria usually cause sexually transmitted infections?
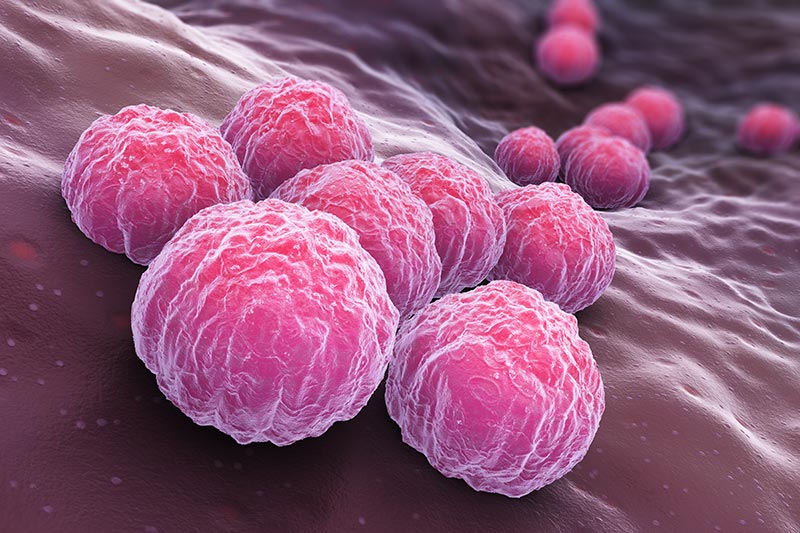
The most common STIs are caused by bacteria including chlamydia and gonorrhoea. They are transmitted through unprotected sexual activity. They are often caught by teenagers and young adults.
Chlamydia is the most common bacterial STI in the UK. It is caused by Chlamydia trachomatis which usually infects the genital tract but can also affect the eyes. The genital tract is part of the organs used in reproduction.
Gonorrhoea (sometimes known as “the clap”) is caused by the bacteria Neisseria gonorrhoeae which is usually found in discharge from the penis or vaginal fluid. The bacteria commonly infect the urethra which is the tube that passes urine out of the body. It can also infect the cervix which is the entrance to the womb. In some cases, the rectum can also be infected.
A third bacterial STI caused by Mycoplasma genitalium is less common in the UK than chlamydia or gonorrhoea. This bacteria is sometimes called “Mgen”. Mgen usually infects the urethra, cervix, and womb but in rare cases it can infect the rectum.
What are the symptoms of an antibiotic-resistant sexually transmitted infection?
Symptoms of an STI may take some time to develop. Many people remain asymptomatic for many days. People may not show any signs of infection and are unaware that they have an STI. This means that they can infect other people without knowing. One in 10 of men and almost half of women infected with gonorrhoea will remain symptom free throughout the infection period. In those who do experience symptoms, these symptoms will usually appear within 10 days of the first exposure.
Symptoms can be quite broad and easily mistaken for other conditions such as urinary tract infection or thrush.
Symptoms include:
- Pain when urinating
- Unusual discharge from vagina, penis or anus
- Itching around the genitals or anus
- Pain during sexual intercourse
Are sexually transmitted infections contagious?
If you have an infection of any type, there is always a risk that it could by caught by the people around you if you do not follow proper hygiene standards. Antibiotic resistant STIs are harder to treat. Find out more about what you can do to prevent the spread of harmful bacteria.
Any person who is sexually active can become infected with an STI and pass it onto others. The risk is not linked to a person’s age.
STIs are spread through contact with bodily fluids such as semen or vaginal fluid. They can also be spread through direct contact with mucus membranes including mouth sores.
Contact with infected body fluid or mucus membranes occurs easily during unprotected sexual activity. This includes vaginal, anal and oral sex. Anal sex carries the biggest risk of passing on STIs because the lining of the anus is thin and easily damaged which can result in infection.
Other sexual activity, such as sharing sex toys, can pass on STIs if the toys are not cleaned well between each use.
How are antibiotic-resistant sexually transmitted infections usually treated?
Most STIs are identified and treated outside of a hospital either in sexual health clinics or GP surgeries. Molecular PCR (polymerase chain reaction) tests are used to diagnose STIs rapidly in sexual health clinics.
Gonorrhoea is usually treated with an antibiotic called ceftriaxone. This is injected once only into the muscle of thigh or buttock. This is called an intramuscular injection. It helps if the antibiotic sensitivity of the bacteria is known beforehand, (which means testing which helps identify or choose the drug most likely to effectively treat the bacterial infection). Often a single dose of an antibiotic tablet called ciprofloxacin or azithromycin may work well. Some people may be given a single dose of an oral tablet called cefixime. Other people may be given an intramuscular injection of gentamicin as well as an oral tablet called azithromycin to treat the gonorrhoea.
Chlamydia is usually treated with a short course of oral antibiotic tablets called doxycycline or azithromycin. If these drugs make the person poorly or the side effects are not tolerated then other antibiotic tablets such as erythromycin or ofloxacin can be used in longer courses.
Mgen is also treated with a short course of doxycycline. This may be followed by azithromycin if antibiotic sensitivity of the bacteria causing the infection is known. Some people may be given a course of antibiotic tablets called moxifloxacin instead.
What happens if I have a multidrug-resistant sexually transmitted infection?
Patients who have had a poor clinical response to their first treatment will be screened to exclude multidrug resistant STIs. A poor clinical response means that the drug has not cured the infection. Multidrug resistant STIs are identified by taking vaginal or urethral swabs which are sent for culture (that is, to grow and identify the bacteria) and antibiotic sensitivity testing in a lab. Future drug treatments are guided by the results of the culture and antibiotic sensitivity test.
Multidrug resistant gonorrhoea may be treated with an injectable antibiotic called ertapenem. Multidrug resistant chlamydia may be treated with tablet antibiotics such as erythromycin or azithromycin. Multidrug resistant Mgen may be treated using tablet antibiotics called pristinamycin or minocycline.
How quickly will the infection spread? Is there anything I can do to stop it getting worse?
Most STIs take some time to show symptoms in infected people. It is possible to spread the infection to other people without knowing. This makes the management of STIs particularly challenging. Timely screening, access to sexual health clinics and patient contact tracing are important to stop these infections spreading.
If you think you have caught an STI, you should get yourself tested as soon as possible and wait for the test results before engaging in any further sexual activity.
The best way to prevent an STI is to use condoms during any type of sexual activity and have regular tests.
What do I do if I have a question about antibiotic-resistant infections?
If your question is about your health, please contact your GP or the clinical specialist you have been seeing. In the case of an urgent, out-of-hours change in your condition, call 111 to find out whether you need to attend hospital. If you are experiencing a health emergency, attend your nearest accident and emergency, taking all of your medications with you.
If you are not seeking health advice, but would like to talk to someone who understands antibiotic resistance and can help you find more information or provide a listening ear, get in touch with our Patient Support Officer, Arlene.
Find out more
Explore our website to find out more about antibiotics, bacteria and the common infections they cause, and our research.
Help us make a difference
Antibiotic resistance could affect everyone on the planet, and estimates suggest it will be responsible for 10 million deaths a year by 2050. We are the only charity in the world dedicated to researching this issue, supporting patients affected by resistant infections and educating the public on antibiotic resistance.
Please make a donation or support our work today, and help us ensure a safer future for our children and grandchildren.
Disclaimer: Any medical information referred to in or through our website is given for information purposes only and is not intended: to constitute professional advice for medical diagnosis or treatment; to replace consultation with a qualified medical practitioner; to advocate or recommend the purchase of any product; or to endorse or guarantee the credentials or appropriateness of any health care provider. You are strongly advised to consult with an appropriate professional for specific advice tailored to your situation. Instead, information provided on our website is intended to provide helpful signposting towards further information and support and to provide an opportunity for you to simply share and discuss matters relating to antibiotic resistance with our Patient Support Officer.
